
|
Posted by www.psmbrokerage.com Admin on Fri, Dec 17, 2021 @ 03:47 PM

|
Posted by www.psmbrokerage.com Admin on Fri, Dec 17, 2021 @ 03:09 PM

Many seniors chose not to make a shift during the 2022 open enrollment season because they did not think they could find a health plan better than their current one.Nearly nine out of every ten American seniors had not changed Medicare plans with less than a month left in the 2022 open enrollment season, according to a MedicareGuide.com survey. MedicareGuide.com surveyed over 2,280 seniors over the age of 65 from November 15 through November 17, 2021. At the time of the survey, there were three weeks left in the 2022 Medicare open enrollment season. “Historically, most beneficiaries don’t change plans, but coverage and cost can change significantly year to year, especially now because of Covid,” said Jeff Smedsrud, the co-founder of HealthCare.com, MedicareGuide’s parent company. “It is becoming easier to use online tools to review your plan and find potential savings. It pays to shop around.”
These results sync with a previous survey which found that, while the coronavirus pandemic caused many younger Americans to consider changing their health plans, older Americans were reticent to do so. Seniors noted a handful of reasons why they chose not to change Medicare Advantage plans. Most seniors who did not change health plans (67 percent) said that they could not find a better health plan than the one that already covered them. Nearly one in five seniors said that they did not change health plans because they would not have saved on their premiums. Cost seemed to be a major factor in seniors' health plan selection process in 2022. Zero-dollar premium Medicare Advantage plans have gained in popularity, driving down the average health plan premium to $4 per month. However, most beneficiaries who did switch plans and found a plan with a lower premium (85 percent) saved between $0 and $50 each year. Another 18 percent of seniors did not change health plans because they found the process overwhelming. Lack of healthcare literacy and general confusion about the health plan selection process are perennial problems during open enrollment season. According to a survey commissioned by GoHealth, almost four in ten beneficiaries found Medicare resources confusing. Eleven percent of all respondents switched to Medicare Advantage from Original Medicare, primarily due to Medicare Advantage’s benefits. The hesitance to change health plans is not new. Most beneficiaries have never switched health plans before (66 percent). Eighteen percent reported that they had changed health plans one time. Even more beneficiaries (85 percent) reported that they did not change their prescription drug health plan during the 2022 open enrollment season. For 9 percent of those who changed their prescription drug plans, pricing was the primary driver. Seniors also prioritized supplemental benefits. Fifteen percent of respondents were looking for dental, hearing, and vision benefits, while 13 percent sought improved drug coverage. Medicare Advantage plans and advocates have pushed to protect supplemental benefits in Medicare Advantage. For example, Better Medicare Alliance made several recommendations to CMS regarding how to preserve supplemental benefits in order to enhance health equity efforts in the senior patient population. Although supplemental benefits have been marked as a unique strength of Medicare Advantage coverage, these benefits in Medicare Advantage can still result in out-of-pocket healthcare spending, an analysis from Kaiser Family Foundation found. As a result, policymakers are considering whether to include supplemental benefit coverage in fee-for-service Medicare for services such as hearing and vision. In a letter to Congress, Better Medicare Alliance also stressed the need to structure fee-for-service Medicare benefits in such a way that they do not interfere with Medicare Advantage benefits. Source: https://healthpayerintelligence.com/news/few-seniors-have-changed-plans-during-2022-open-enrollment  |
Tags: Medicare open enrollment, Medicare Advantage plans, AEP
Posted by www.psmbrokerage.com Admin on Mon, Dec 13, 2021 @ 02:03 PM

“This report provides valuable insights into telehealth usage during the pandemic,” said CMS Administrator Chiquita Brooks-LaSure. “CMS will use these insights – along with input from people with Medicare and providers across the country – to inform further Medicare telehealth policies.” “During the COVID-19 pandemic, various telehealth flexibilities enabled patient access to their providers,” said HHS Acting Assistant Secretary for Planning and Evaluation Rebecca Haffajee. “Pre-pandemic telehealth visits for Medicare beneficiaries went from hundreds of thousands to tens of millions, with many utilizing telehealth for the first time. Today’s report offers a detailed data analysis on important trends for policymakers.” To help beneficiaries maintain some access to care amid stay-at-home orders to reduce COVID-19 related exposure, CMS used emergency waiver authorities enacted by Congress, as well as existing regulatory authorities to implement policies expanding access to telehealth services during the pandemic. These included waiving several statutory limitations such as geographic restrictions and allowing beneficiaries to receive telehealth in their home. Outside of the public health emergency (PHE), Medicare is generally restricted to payment for telehealth services in certain, mostly rural areas, and when beneficiaries leave their home and go to a clinic, hospital, or other type of medical facility for the service. There were some exceptions for beneficiaries with end-stage renal disease, stroke and other specific conditions. Additionally, in response to the pandemic, the HHS Office for Civil Rights relaxed enforcement of Health Insurance Portability and Accountability Act (HIPAA) of 1996 privacy requirements for videoconferencing. Taken as a whole, the ASPE report found that the share of Medicare visits conducted through telehealth in 2020 increased 63-fold, from approximately 840,000 in 2019 to 52.7 million. States with the highest use of telehealth in 2020 included Massachusetts, Vermont, Rhode Island, New Hampshire and Connecticut. States with the lowest use of telehealth in 2020 included Tennessee, Nebraska, Kansas, North Dakota and Wyoming. The report also found insightful trends on the kinds of services Medicare beneficiaries sought through telehealth. While overall health care visits for Medicare beneficiaries declined in 2020 as compared to 2019, telehealth was particularly helpful in offsetting potential foregone behavioral health care. In 2020, telehealth visits comprised a third of total visits to behavioral health specialists, compared to 8 percent of visits to primary care providers and 3 percent of visits to other specialists. These findings prominently show an increased interest in seeking behavioral health care through telehealth. To help protect access to care as informed by data, CMS recently announced that for the first time outside of the COVID-19 PHE, Medicare will pay for mental health visits furnished by Rural Health Clinics and Federally Qualified Health Centers via interactive video-based telehealth, including audio-only telephone calls. Additionally, CMS is permanently eliminating geographic barriers and allowing patients in their homes to access telehealth services for diagnosis, evaluation, and treatment of mental health disorders, including via audio-only communications technology. These provisions were included in the Consolidated Appropriations Act of 2021. Other Medicare services added to the telehealth services list temporarily during the PHE will remain in place through December 31, 2023, while CMS continues to evaluate whether these services should be permanently added to the Medicare telehealth services list. And to provide more transparency and visibility into telemedicine usage, CMS is also releasing a new snapshot showing the number of people with Medicare who utilized telemedicine services between March 1, 2020 and February 28, 2021. The snapshot includes Medicare FFS claims data, Medicare Advantage (MA) encounter data, and Medicare enrollment information. While utilization of telehealth services increased and improved access to services for many beneficiaries, more research is needed to understand the impact on quality of care and why certain beneficiaries used less telehealth than others.
 |
Tags: Telehealth
Posted by www.psmbrokerage.com Admin on Tue, Nov 30, 2021 @ 10:37 AM

Relationships are essential for a successful business and Insurance most certainly is a Relationship-based business.
In this video we discuss some of the most important relationships you will have in your insurance business.
We'll share a few insights on how to build and maintain good relationships, because, as you know, it’s not all about what you know, but who you know.
Invest in the right relationships in your business and you will see the results pay off quickly.
[Click the image to watch the video]
We are going to discuss the following 8 Levels of Insurance Relationships:
1. The state (Dept. of Insurance)
2. Your upline
3. Insurance Companies
4. Prospects and Customers
5. Vendors
6. Referral Partners
7. Colleagues
8. Your downline
Make the best of your business relationships and you will increase your chance for business success.
Additional Content:
Top 10 Marketing Ideas for Insurance Agents
7 Ways to Grow Your Insurance Business
Social Media Strategy for Insurance Agents
Posted by www.psmbrokerage.com Admin on Mon, Nov 29, 2021 @ 04:40 PM
10 Cities. 9 Months. 8% Roadshow.How do successful people think? From the professional to the personal realm, hear how you can better overcome challenges and develop a winning mindset. A destination without a path is unreachable. Learn what leaders from your industry and others did to pave their way to your dream lifestyle.
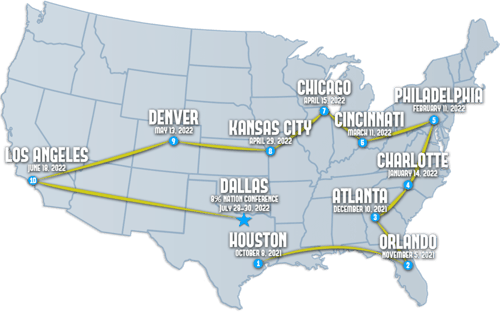 NETWORKINGHave you ever heard the term, “It’s not what you know, it’s who you know?”One of the greatest things about the 8% Nation conference is the attendees themselves. Friendships, partnerships, and mentorships have all happened from agents just like yourself who happened to bump into the right person in the audience. By connecting with the person to your left or your right (or both) at our conference, you can hold each other accountable to your new goals, challenge yourselves to do more every day, and help each other to keep a growth mindset. It’s important to keep successful people around you if you want to achieve your goals and the people who attend 8% Nation are the ones who are committed to doing something big with their lives.  |
|||
Tags: Success Tips, Professional Networking, sales advice, Entrepreneurship, Insurance Marketing, Leadership
Posted by www.psmbrokerage.com Admin on Mon, Nov 29, 2021 @ 03:49 PM

Agents can now qualify for a bonus beginning with their first sale during AEP. All Agents have access to more this AEP with Humana Achieve bonus incentives.
 |
Tags: Bonus Program, Humana Achieve

⭐ Additional benefits include:
If you have any questions about the YourMedicare Telephonic Enrollment platform, please contact us at 800-998-7715 for more details and training. 👉 YourMedicareBot Registration Page 👉 YourMedicareBot Portal Login Page 👉 YourMedicareBot Training Videos  |
Tags: Medicare Advantage, Enrollment Tools, MyMedicareBot, Voice Signature

And while the survival rate is increasing, the cost to treat cancer is also increasing, up 27% since 2011 according to Health Leaders Media. In this short video we will cover some of the common costs of cancer as well as some misconceptions that people have regarding these costs and how their current insurance plan will provide coverage.
Some additional facts on cancer to consider. The median age of a cancer diagnosis is 66. Half of cancer cases occur in people younger than 66. One-quarter of new cancer cases are diagnosed in people aged 65 to 74. Cancer can occur at any age. For example, bone cancer is most frequently diagnosed among people under age 20. More than one-fourth of cases occur in this age group. The median age at diagnosis is 61 years for breast cancer, 68 years for colorectal cancer, 70 years for lung cancer, and 66 years for prostate cancer. Cancer is the #1 reason for claims made by individuals with critical illness insurance. It accounts for between 50 and 64 percent of claims. This valuable protection pays a lump-sum cash payment. The monies are paid directly to the policyholder. They can be used to cover any costs you face. You may also choose to get a cancer-only insurance policy. That can save you money on valuable protection.  |
Tags: cancer insurance
.png?width=625&name=happy%20Thanksgiving%20(1).png)
Posted by www.psmbrokerage.com Admin on Mon, Nov 15, 2021 @ 03:23 PM

With 55-60% of enrollments typically completed in the last five weeks of AEP, efficiency and personalization will be key to engaging with more prospects and existing members.
Click on the link below to start enrolling your Medicare clients over the phone. Activation Code: yourmedicareagent2022
Resources: 👉 YourMedicareBot Resource Page👉 YourMedicareBot Registration Page 👉 YourMedicareBot Portal Login Page 👉 YourMedicareBot Training Videos
 |
|||
Tags: Humana, Medicare Advantage, aetna, Enrollment Tools, MyMedicareBot, Voice Signature
©2024 Precision Senior Marketing | 11940 Jollyville Rd #200 South, Austin TX 78759 | Phone: (800) 998-7715
*“Not affiliated with the U. S. government or federal Medicare program. This website is designed to provide general information on Insurance products, including Annuities. It is not, however, intended to provide specific legal or tax advice and cannot be used to avoid tax penalties or to promote, market, or recommend any tax plan or arrangement. Please note that PSMBrokerage, its affiliated companies, and their representatives and employees do not give legal or tax advice. Encourage your clients to consult their tax advisor or attorney.