|
Medicare Part B Premium and Deductible Medicare Part B covers physician services, outpatient hospital services, certain home health services, durable medical equipment, and certain other medical and health services not covered by Medicare Part A. Each year the Medicare Part B premium, deductible, and coinsurance rates are determined according to the Social Security Act.
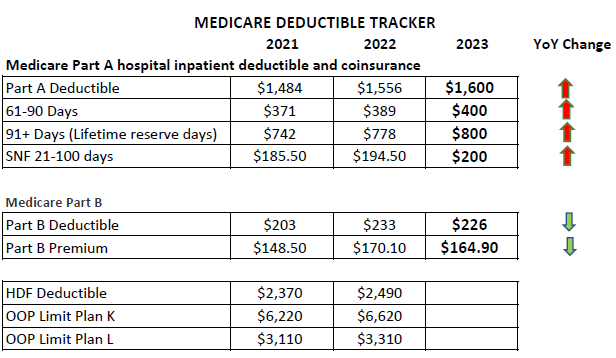
The 2022 premium included a contingency margin to cover projected Part B spending for a new drug, Aduhelm. Lower-than-projected spending on both Aduhelm and other Part B items and services resulted in much larger reserves in the Part B account of the Supplementary Medical Insurance (SMI) Trust Fund, which can be used to limit future Part B premium increases. The decrease in the 2023 Part B premium aligns with the CMS recommendation in a May 2022 report that excess SMI reserves be passed along to people with Medicare Part B coverage. Beginning in 2023, certain Medicare enrollees who are 36 months post kidney transplant, and therefore are no longer eligible for full Medicare coverage, can elect to continue Part B coverage of immunosuppressive drugs by paying a premium. For 2023, the immunosuppressive drug premium is $97.10. Medicare Open Enrollment and Medicare Savings Programs Medicare Open Enrollment for 2023 will begin on October 15, 2022 and ends on December 7, 2022. During this time, people eligible for Medicare can compare 2023 coverage options between Original Medicare, and Medicare Advantage, and Part D prescription drug plans. In addition to the soon-to-be released premiums and cost sharing information for 2023 Medicare Advantage and Part D plans, the Fee-for-Service Medicare premiums and cost sharing information released today will enable people with Medicare to understand their Medicare coverage options for the year ahead. Medicare health and drug plan costs and covered benefits can change from year to year, so people with Medicare should look at their coverage choices annually and decide on the options that best meet their health needs. To help with their Medicare costs, low-income seniors and adults with disabilities may qualify to receive financial assistance from the Medicare Savings Programs (MSPs). The MSPs help millions of Americans access high-quality health care at a reduced cost, yet only about half of eligible people are enrolled. The MSPs help pay Medicare premiums and may also pay Medicare deductibles, coinsurance, and copayments for those who meet the conditions of eligibility. Enrolling in an MSP offers relief from these Medicare costs, allowing people to spend that money on other vital needs, including food, housing, or transportation. People with Medicare interested in learning more can visit: https://www.medicare.gov/your-medicare-costs/get-help-paying-costs/medicare-savings-programs. Medicare Part B Income-Related Monthly Adjustment Amounts Since 2007, a beneficiary’s Part B monthly premium is based on his or her income. These income-related monthly adjustment amounts affect roughly 7 percent of people with Medicare Part B. Medicare Part A Premium and Deductible Medicare Part A covers inpatient hospital, skilled nursing facility, hospice, inpatient rehabilitation, and some home health care services. About 99 percent of Medicare beneficiaries do not have a Part A premium since they have at least 40 quarters of Medicare-covered employment. The Medicare Part A inpatient hospital deductible that beneficiaries pay if admitted to the hospital will be $1,600 in 2023, an increase of $44 from $1,556 in 2022. The Part A inpatient hospital deductible covers beneficiaries’ share of costs for the first 60 days of Medicare-covered inpatient hospital care in a benefit period. In 2023, beneficiaries must pay a coinsurance amount of $400 per day for the 61st through 90th day of a hospitalization ($389 in 2022) in a benefit period and $800 per day for lifetime reserve days ($778 in 2022). For beneficiaries in skilled nursing facilities, the daily coinsurance for days 21 through 100 of extended care services in a benefit period will be $200.00 in 2023 ($194.50 in 2022).
 |
Medicare Blog | Medicare News | Medicare Information
2023 Medicare Parts A & B Premiums and Deductibles
Posted by www.psmbrokerage.com Admin on Thu, Sep 29, 2022 @ 10:13 AM
|
|
Tags: Medicare Part A, Medicare Part B, 2023
2022 AAHU Golf Tournament Recap
Posted by www.psmbrokerage.com Admin on Wed, Sep 28, 2022 @ 11:19 AM
|
PSM was a proud sponsor of this years AAHU Golf Tournament held at Balcones Woods country club in Austin. It was a wonderful event and a great opportunity to network with other insurance professionals and discuss the changes shaping our industry. We appreciate all those who attended and contributed and can't wait for next years event!
 |
|||
Tags: AAHU
YourMedicare SunFire Daily Webinars
Posted by www.psmbrokerage.com Admin on Wed, Sep 28, 2022 @ 10:24 AM
|
YourMedicare SunFire Daily Webinars Starting this Wednesday, YourMedicare will be hosting daily webinars specifically going over the new call recording technology in YourMedicare SunFire. They will all be at 2:00 EST. YourMedicare will cover the setup process, how to use the new feature and answer all of your questions! This is a reoccurring event so there is no registration required. Join us every Wednesday at 2:00 EST. You can also learn more by attending one of our weekly webinars. View schedule
 |
Tags: Medicare Advantage, AEP, SunFireMatrix, Compliance, MyMedicareBot, call recording
Sunfire: Telephony System is LIVE!
Posted by www.psmbrokerage.com Admin on Fri, Sep 23, 2022 @ 09:56 AM
|
YourMedicare SunFire users, Today is the day! Be sure to log in and establish your new virtual phone number. Here is a step-by-step guide:
To register for a webinar go to https://yourmedicareresources.com/webinars/ To register for the SunFire Platform, request details here.
New CMS Requirement
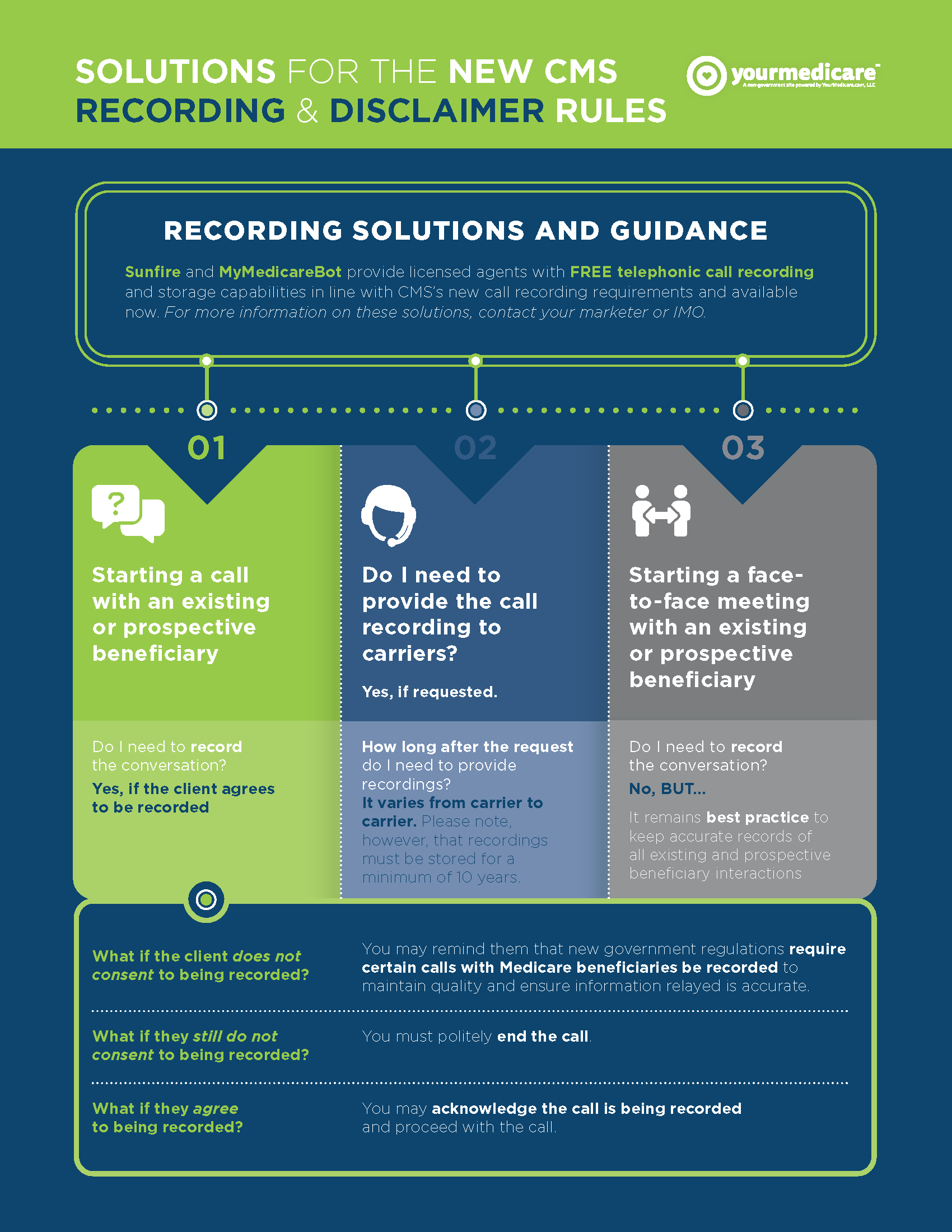
Effective October 1, 2022 Field Agents will be required to record all sales and marketing calls in their entirety. The recordings must be retained in a HIPAA compliant manner for 10 years. View details on the new CMS rule here.
This pertains to calling leads, scheduling appointments, collecting drug and provider lists and conducting phone enrollments. 
Only in person, face to face appointments are excluded, however any follow up calls related to sales and completing the enrollment process must be recorded.
Additionally, a new disclaimer must be verbally conveyed within the first minute of a sales phone call.
Now is a great time to make sure you have access to Sunfire's enrollment platform and have a solution in place for the upcoming 2023 AEP.
 |
|||
Tags: Medicare Advantage, CMS, AEP, SunFireMatrix, Compliance, 2023
American Home Life Patriot Series | Now Available in FL & PA
Posted by www.psmbrokerage.com Admin on Fri, Sep 23, 2022 @ 09:05 AM
|
Great news! Effective today, agents are now able to offer AHL’s Medicare Supplement & Patriot Series Final Expense plans in Florida & Pennsylvania!
Whether your client needs Final Expense or Medicare Supplement, American Home Life has exactly what they need. Our Patriot Series Final Expense product is available to provide flexible coverage to meet your client's unique needs and our Medicare Supplement product offers Plans A, F, G, and N with varying amounts of coverage. Patriot Series Final Expense The Patriot Series Final Expense offers 4 plans to best meet your clients needs. Three level plans and one modified plan are all available with flexible coverage options. Medicare Supplement The American Home Life Insurance Company also offers Medicare Supplement plans. Plan A provides basic benefits, while Plan F offers more comprehensive coverage. With more tools for agents, and benefits for customers, this offer is almost two good two be true. Request product details and contracting today.
American Home Life's "Shoot for the Stars" Producer Incentive Program is now live! To earn your $500 , all you have to do is write at least four policies before October 14th.
 |
|||
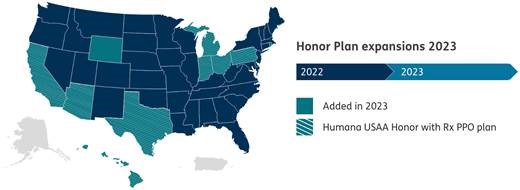
Attention: Humana Introducing the new 2023 Honor Plans
Posted by www.psmbrokerage.com Admin on Thu, Sep 22, 2022 @ 03:37 PM
|
Serving those who've served Humana’s long-standing support of our nation’s active-duty military and veteran communities dates back decades. It’s why we continue to make veteran health and wellness a priority. That dedication to service helped us earn USAA’s recommendation on our 2023 Medicare Advantage plans. And it’s why we worked with USAA to develop the all-new Humana USAA Honor with Rx plan especially designed with veterans in mind and available to anyone eligible for Medicare. These plans complement and work alongside benefits that veterans may receive from the VA.
Hold onto your hats—our 2023 Humana Honor Plan news is big. Check it out.
*As a reminder, agents are prohibited from marketing or communicating 2023 plan information prior to Oct. 1.
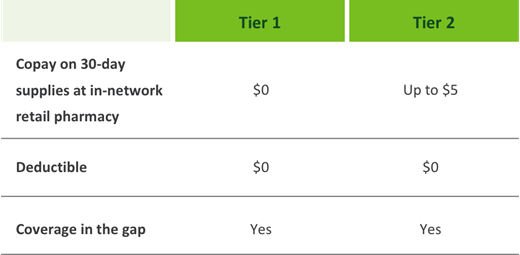
 Discover the new Humana USAA Honor with Rx plan in 8 states Specially designed in collaboration with USAA, this new $0 premium Medicare Advantage plan with prescription drug coverage helps beneficiaries get the coverage they need at the doctor and the pharmacy. It was built to meet the unique needs of veterans, and it's available to anyone eligible for Medicare. Prescription coverage
Additional features that make this plan unique
Available in 1,095 counties in 8 states The Humana USAA Honor with Rx plan is available throughout Pennsylvania and in select markets in Texas, Michigan, Ohio, Indiana, Arizona, California and Hawaii.
 |
|||
Tags: Humana, Medicare Advantage plans
House passes bill to install electronic prior authorization in Medicare Advantage plans
Posted by www.psmbrokerage.com Admin on Thu, Sep 22, 2022 @ 03:03 PM
|
The House unanimously passed the Improving Seniors’ Timely Access to Care Act on Wednesday via a voice vote. The legislation, which has new transparency requirements for MA plans, now heads to the Senate. Lawmakers behind the legislation said in a joint statement the bill will “make it easier for seniors to get the care they need by cutting unnecessary red tape in the healthcare system,” said Reps. Suzan DelBene, D-Washington, Mike Kelly, R-Pennsylvania, Ami Bera, M.D., D-California, and Larry Bucshon, M.D., R-Indiana. Prior authorization—where providers must first get insurer approval before performing certain services or making prescriptions—has increased in recent years much to the chagrin of providers who charge the process causes a massive administrative burden.
The House bill aims to require the establishment of an electronic prior authorization process for all MA plans to hasten the approval of requests. It would also require the Department of Health and Human Services (HHS) to create a process for faster, “real-time” decisions on the items or services that already get routinely approved.
Another new requirement is that MA plans must report to the federal government on how they use prior authorization, as well as the rate that such requests are approved and denied. The requirement comes as HHS’ watchdog found that MA plans have denied prior authorization claims for services that met Medicare’s coverage requirements. The overwhelming House vote earned plaudits from several provider groups. “At a time when group practices face unprecedented workforce shortage challenges, 89% of [Medical Group Management Association] members report they do not have adequate staff to process the increasing number of prior authorizations from health insurers,” the Medical Group Management Association said in a statement. “By streamlining and standardizing the overly cumbersome and wildly inefficient MA prior authorization process, this legislation will return a focus to the physician-patient relationship.”  |
|||
Tags: Medicare Advantage plans
|
You work hard all year, but especially during the AEP/OEP season. We would like to show our appreciation for your dedication to Ameritas and our individual dental products with this bonus program. Program details:

 |
||||
Tags: ameritas, dental plans, Incentives
|
WIN BIG Sell Medicare Supplement policies with American Benefit Life and Capitol Life, and you could win big. The more qualified applications you submit, the more you can earn. At the conclusion of the contest period, select your prize – a trip to Las Vegas or a cash payout.
Feeling lucky? Contact us at 800-998-7715 to learn how you can win big.
 |
|||
Commentary: CMS Medicare recording requirement could risk senior data
Posted by www.psmbrokerage.com Admin on Wed, Sep 14, 2022 @ 10:55 AM
|
By Joshua Brooker Starting Oct. 1, the Centers for Medicare and Medicaid Services will require health insurance agents and brokers to record all Medicare-related phone calls. At face value, having a recording of a call sounds like a great way to catch bad actors who misinform seniors about their options pertaining to Medicare. Here is my question to you, though: If I were to ask you to start recording all calls tomorrow, and do so securely as well as securely store the calls for 10 years, how would you do it? If your answer is, "I'm not sure," then we have a problem. Because that is exactly what the government is doing. They have advised the insurance agent and broker community, of which there are 100,000 self-employed mom-and-pop agencies across the country helping Americans, to record all calls but provided no guidance or support to do so. Why is this happening?Whether an individual is nearing age 65, or already has been on Medicare for years, there is no denying the onslaught of information they receive every day about Medicare, the plans they have access to, and the push for them to "act now.” According to the Federal Registry, in 2022, CMS reported 39,617 "complaints to Medicare" related to misinformation. This is out of 29 million enrollments. This represents only 0.0013661% of the total enrollments made during the most recent open enrollment period. Even though the complaints represent such a small number of seniors overall, CMS is trying to make strides toward fixing two things:
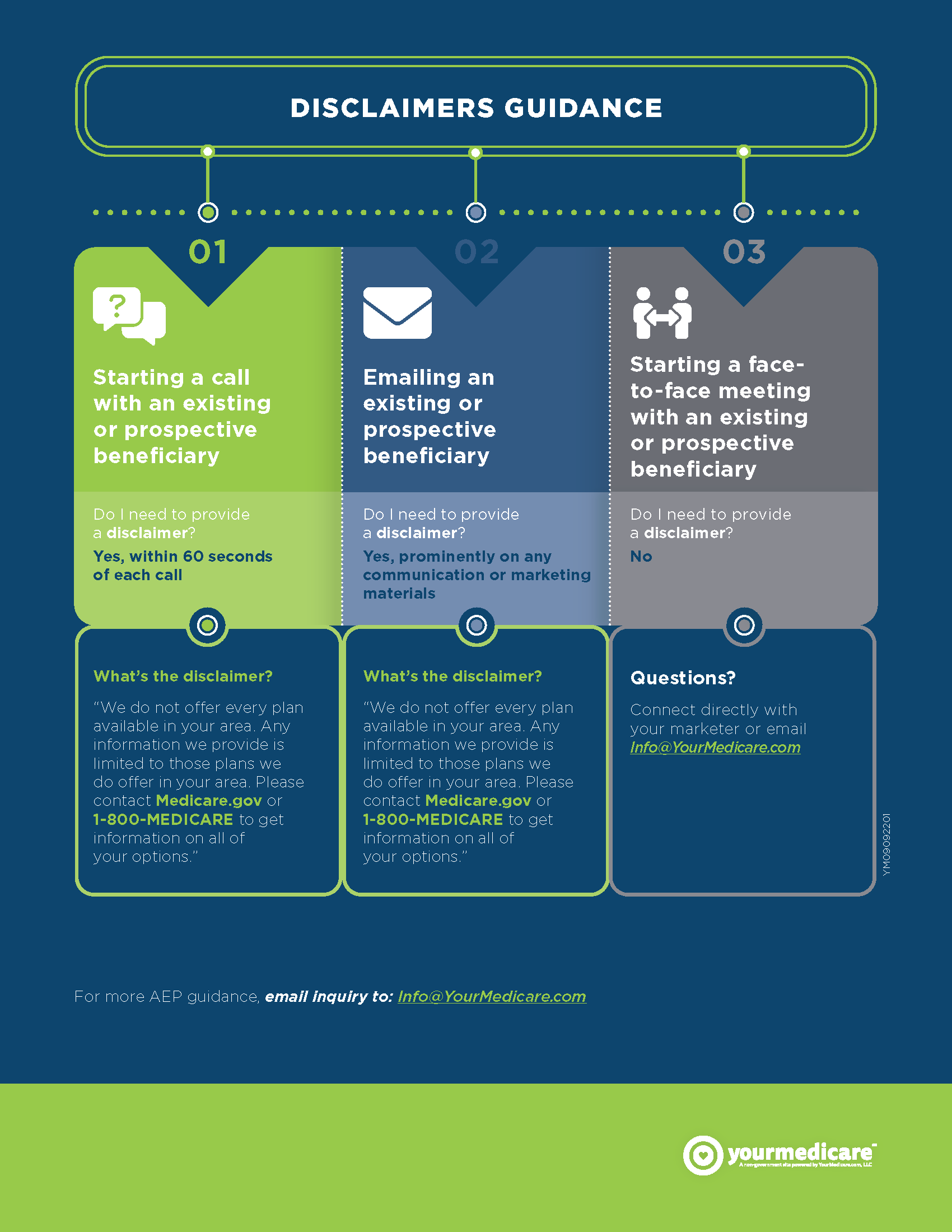
Consumers want to know who will receive their information upon filling out a form online or calling a toll-free number. Consumers also want to be confident that the broadest amount of plans are considered before a recommendation is made. CMS solution: proactive disclosureIn an effort to address Concern No. 1, CMS is requiring all marketing companies, as well as agents and brokers to state on their website and in the first 60 seconds of each phone call that "We do not offer every plan available in your area. Any information we provide is limited to those plans we do offer in your area. Please contact Medicare.gov or 1-800-MEDICARE to get information on all of your options." When a senior wants a local representative who is licensed in their state, certified to talk about Medicare, and understands the nuances of the local health systems and insurance plan options, they are looking for a resource beyond Medicare.gov and/or 1-800-MEDICARE. This disclosure does not address seniors’ underlying concerns. Another issue with this disclosure is that it doesn't tell the consumer whether the person on the line is a tethered/captive insurance agent, a marketing/lead generation company, or an untethered independent broker. Nor does it tell consumers the scope of options available to the consumer. If a given county has 70 plans available, and the person on the other end of the line has access to three plans, I think that there is a cause for disclosure. That said, some plans tied to special needs, only available only to captive agents might cause someone to have 65 plans available. Both scenarios require the same disclosure, and while the former (three plans) is alarming, the latter (65 plans) is understandable. CMS solution: call recordingAlthough CMS is hopeful that disclosure will inform individuals about their options, the agency also requires all tethered and untethered agents as well as lead generation companies to record calls. Actually, tethered agents tied to insurance company call centers, and lead generation companies already have this requirement. The May 9, 2022, rule added independent, untethered brokers to this recording requirement. Related Article: Call Recording Making Your Head Spin? As we have discussed, independent brokers are untethered insurance brokers who have the broadest plans from which to make recommendations, are licensed to interpret insurance laws, and do not operate as middlemen who sell your information like lead generators for other tethered or insurance companies. Untethered brokers are small businesses entrenched in their communities whose clients come from many sources, such as current clients, other insurance brokers, financial advisors, employers and human resource directors. Issue #1: small business requirements According to the Bureau of Labor Statistics, a broker's median wage is $49,840 per year. They aren't the upper crust of the insurance industry who can receive seven-figure salaries. Rather, as an individual in their community, they are being required to seek and deploy software to record all calls related to Medicare. The government failed to consider the limited resources of these individuals, and neither larger agencies nor insurance companies are tasked with providing support. Instead, the burden falls on the individual broker who must find software, set it up, record all calls, store all calls and make them available to regulators at a moment's notice, all while being secure in the process. When laws are passed by government agencies, if they are a burden to small businesses, they must make accommodations for those entities that are impacted the most. Not only are they adding a burden for the broker community to add compliant software, but they are also requiring that same agent or broker to tell every person they speak to on the phone to get their needs met elsewhere (medicare.gov and 1-800-MEDICARE). Issue #2: risking senior data Another issue to consider is the likelihood of compromised senior data. Alissa Knight, a partner at Knight Ink Media, is a chief information security officer and cybersecurity expert. She was a keynote speaker at a national Health Information and Management Systems conference. On a recent podcast, she said, "Electronic health records are worth 1,000 times more than a U.S. credit card number." She went on to explain, that if your credit card is stolen, your bank can send you a new card and you're fine. If your health history is compromised (accessed from one of these storage sites) and put on the dark web to sell, "how easy it is to get new health history sent to you in the mail? You can't. It's gone. If I want to figure out how to kill Larry, I find his protected health information, and I find out he is allergic to bee stings, I go after him with some bumblebees." In a phone call, not only might a recording include information about the individual on the phone, but seniors routinely talk about their spouses, kids, grandkids and other individuals. All of these could open up calls to not one, but multiple data points being at risk. Knight said health data is "such a lucrative business to be in." Obviously, she is looking at ransomware attacks. She goes on to state, that if a hacker is "targeting something like a Cerner EHR system [like data stored by a hospital or insurance company], that may be very well protected and very secure." If there is a less secure system outside of these secure programs, "where do you think I'm going to target as a hacker? I'm going to target the less secure. I'm going after the path of least resistance." Medicare represents more than 60 million seniors. Without defined policy and infrastructure in place, brokers are the path of least resistance. With 100,000 agents and brokers trying to figure out how to comply, this risk for anyone is dangerous. The current requirement to record calls is in the spirit of helping beneficiaries. We worry that the risk of senior data being exposed egregiously outweighs the risks of not recording calls. RecommendationsFirst, we'd like to address the spirit of the law. As independent brokers who have more than 50 insurance company contracts, and are entrenched in our community, we stand by regulations that serve the consumer’s best interest. At the end of the day, we often must address the same misinformation and complaints that Medicare deals with directly, and we work on the front lines to get Medicare right. This is why we are commenting on this rule. And, rather than pointing fingers, we offer real-world solutions.
Some tethered contracts require the agent to not get appointed to plans not available through the insurer, or their dedicated system. These clauses should be known to help identify tethered entities. This rework would tell the consumer who is receiving their data and which options the company is presenting against the total options of the market. Joshua Brooker, REBC, ABHP, ASFC, is principal at PA Health Advocates, Lancaster, Pa. He is a member of the National Association of Health Underwriters and Health Agents for America.
 |
|||||
Tags: CMS, Compliance, call recording